Alveolar Rhabdomyosarcoma Cancer
Alveolar rhabdomyosarcoma (ARMS) is a rare childhood cancer of soft tissues, and whereas this disease often responds to chemotherapy initially, metastatic patients eventually fail all available treatments — a deadly outcome.
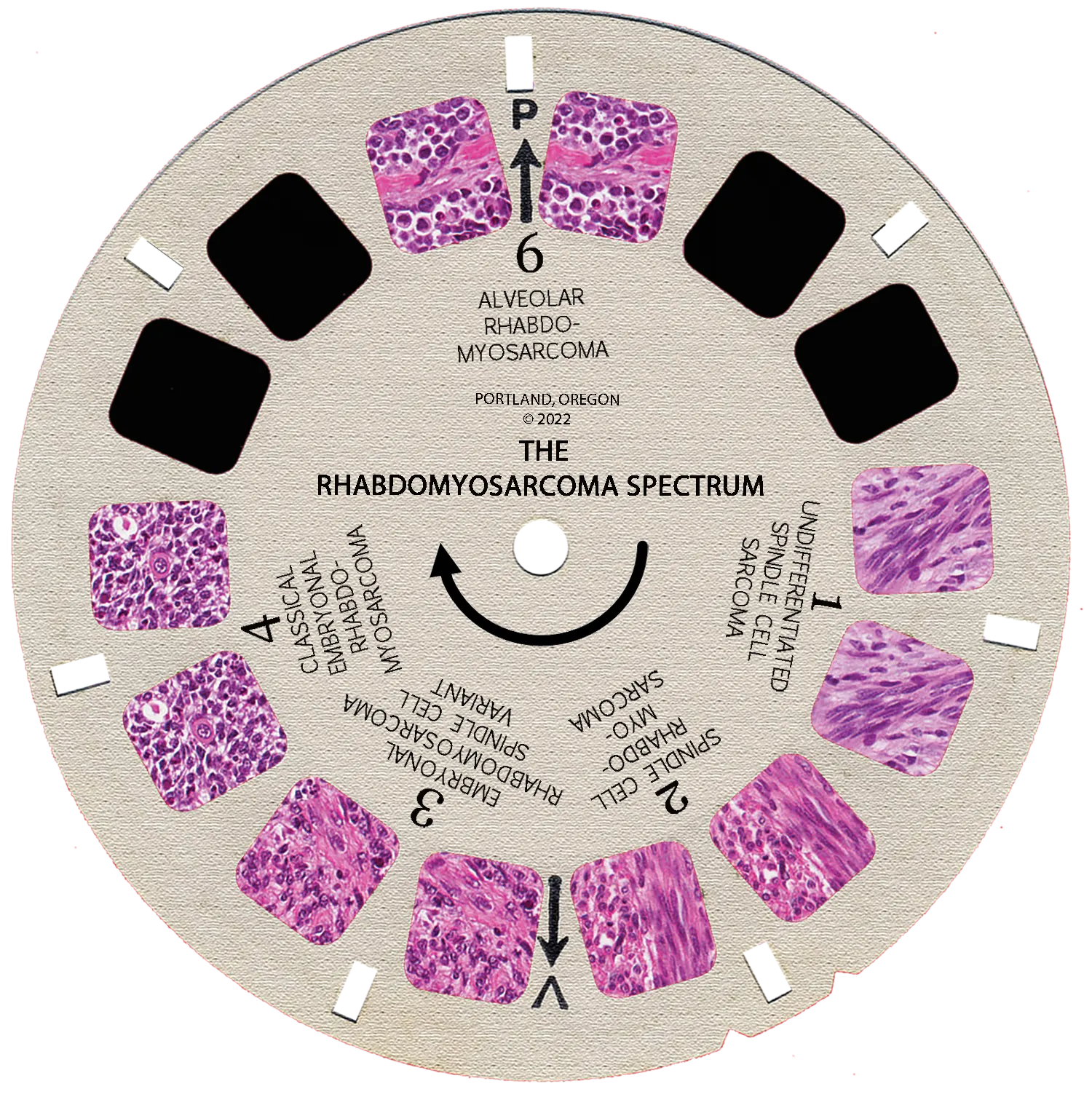
Alveolar Rhabdomyosarcoma Cancer
Uncurable childhood cancer
Alveolar rhabdomyosarcoma is an aggressive form of childhood cancer that arises in muscle tissue. While some cases can be treated when localized, it becomes extremely difficult to cure once it has spread (metastasized) to other parts of the body.
Metastatic disease means cancer cells have already traveled through the blood or lymph system and formed tumors in multiple locations. This makes complete surgical removal impossible and reduces the effectiveness of radiation. At the same time, the cancer often develops resistance to chemotherapy over time. Because the disease is biologically aggressive and spreads early, current treatments can sometimes control it temporarily—but rarely eliminate it entirely when metastatic.
This combination of widespread disease, treatment resistance, and high relapse rates is why metastatic alveolar rhabdomyosarcoma is still considered largely incurable with today’s standard therapies.
Alveolar Rhabdomyosarcoma Cancer
The Fusion Protein
We identified how a cancer-causing fused protein called PAX:FOXO1 leads to treatment failure. The goal of our drug development program is to create clinical medicines that inactivate the PAX3:FOXO1 and PAX7:FOXO1 ARMS proteins so that the patient can become disease-free.
We have published that expression of the PAX3::FOXO1 oncogene in the G2 phase of the cell cycle facilitates checkpoint adaptation in Fusion+ RMS (manifest as high tolerance of DNA breaks or mitotic catastrophe). This finding correlates with clinical observations showing that the PAX3::FOXO1-mediated treatment resistance causes a notable 40% difference in survival over 10 years compared to PAX3::FOXO1 negative cases. In our experimental studies, knockdown of PAX3::FOXO1 improves chemotherapy & radiation sensitivity and reduces tumor re-establishment.
Furthermore, over a period of several weeks PAX3::FOXO1 appears to be a dependency when expression goes to absolute zero using CRISPR, opening the possibility that PAX3::FOXO1+ RMS may be potentially “curable” with a very efficient PAX3::FOXO1 targeted drug.

